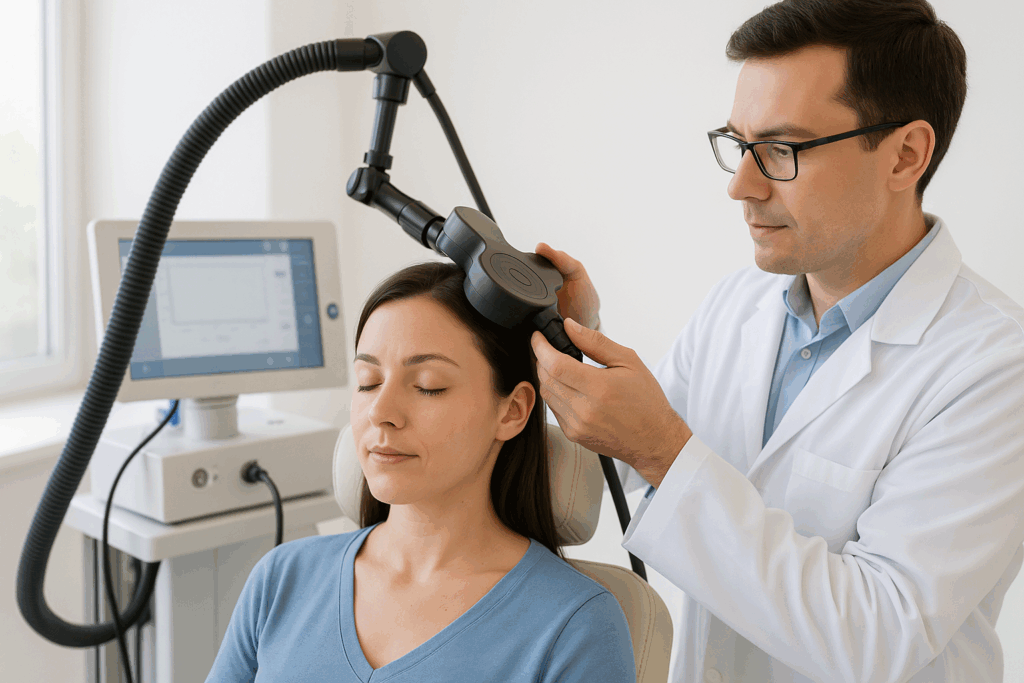
TMS therapy benefits include significant relief from depression without medication side effects, no need for anesthesia or sedation, a strong safety profile backed by FDA clearance, and results that last months to over a year for many patients. According to Harvard Health, approximately 50% to 60% of people with depression who did not respond to medication experience a meaningful response to TMS, and about one-third of those patients achieve full remission. For the millions of Americans living with treatment-resistant depression, TMS therapy offers a proven, drug-free path forward. In this article, we explain what TMS is, how it works, who it helps, what the experience feels like, and how long the benefits last.
What Are the Positive Effects of TMS Therapy?
The positive effects of TMS therapy include improved mood, reduced feelings of hopelessness, better concentration, more energy, improved sleep, and a renewed ability to enjoy activities that depression had taken away. These improvements happen because TMS directly stimulates areas of the brain involved in mood regulation, specifically the dorsolateral prefrontal cortex (DLPFC), which is often underactive in people with depression.
A literature review published in the journal Cureus found that response rates to TMS range between 50% and 55%, with remission rates between 30% and 35% in patients with major depression. A multicenter observational study involving 307 patients confirmed statistically significant improvement in depression severity after TMS treatment. Yale Medicine reports that about 60% of people who did not respond to other depression treatments respond to standard TMS protocols, and more than half of those patients stay in remission at six-month follow-up appointments.
Beyond the numbers, the real benefit is what patients describe: feeling like themselves again. We see this regularly with our patients. After weeks of feeling stuck, they start sleeping better, engaging with their families, and returning to the routines that depression had pulled them away from.
How Does TMS Therapy Work?
TMS therapy works by placing an electromagnetic coil on the scalp that delivers short, focused magnetic pulses to the DLPFC. These pulses stimulate nerve cells in the brain that are underactive in people with depression, essentially helping to reset dysfunctional brain patterns and restore normal mood regulation.
According to UT Southwestern Medical Center, TMS increases neuroplasticity, which is the brain's ability to form new pathways. This allows patients to break out of the depressive patterns that have kept them stuck. The magnetic pulses used in TMS are similar in strength to those of an MRI machine, but they are extremely brief. UCLA Health notes that the total magnetic exposure over a full course of TMS therapy is actually less than the exposure from a single MRI scan.
Each session lasts about 20 to 40 minutes, and patients are awake and alert throughout the entire treatment. There is no anesthesia, no sedation, and no recovery time. You can drive yourself to and from appointments and return to your normal activities immediately after each session. Most treatment courses run five days a week for four to six weeks. Proper psychiatric care includes determining the right treatment intensity and brain target for each individual patient.
What Are the Signs That TMS Is Working?
The signs that TMS is working include improved sleep, more energy during the day, better ability to concentrate, less irritability, a gradual return of interest in activities, and a lifting of the heavy, flat feeling that depression creates. These changes often happen gradually over the first two to three weeks of treatment.
A study from UCLA Health published in Psychiatry Research found that early improvements reported within the first five to ten treatments were significant predictors of how well a patient would respond throughout the full course of treatment. That means your provider can often tell within the first couple of weeks whether TMS is on the right track for you. If progress is slower than expected, adjustments can be made to the treatment protocol.
Most patients do not wake up one day feeling completely different. Instead, the change is gradual. Sleep and appetite tend to improve first. Then energy and focus get better. Mood is usually the last thing to fully lift. It is important to stay consistent with your treatment schedule and to communicate openly with your provider about how you are feeling along the way.
Is TMS Better Than Antidepressants?
TMS is better than antidepressants for many patients, particularly those who have not responded to medication or who experience intolerable side effects. While first-line antidepressants like SSRIs help roughly 40% to 60% of patients, TMS response rates reach 50% to 80% depending on the protocol and patient profile. TMS also avoids the systemic side effects that come with medication, such as weight gain, sexual dysfunction, nausea, and fatigue.
The AAFP (American Academy of Family Physicians) notes that antidepressants are the most commonly prescribed medications for U.S. adults aged 20 to 59. But the NIMH acknowledges that finding the right medication often requires trial and error, and by the time a patient has tried two or three medications without success, the likelihood of the next one working drops significantly. Many patients weighing TMS vs. medication find that TMS fills a critical gap.
It is worth noting that TMS and medication are not mutually exclusive. Many patients use both. Research suggests that patients taking antidepressants while undergoing TMS may actually see better results, because the two treatments can work together. Your provider can help determine whether TMS alone, medication alone, or a combination is the best fit. We often pair TMS with ongoing therapy and medication management for the strongest outcomes.
How Long Do TMS Results Last?
TMS results last six months to a year or longer for most patients who respond to treatment. A systematic review and meta-analysis found that among initial responders, 66.5% sustained their response at three months, 52.9% at six months, and 46.3% at twelve months. A naturalistic one-year follow-up study found that 62.5% of patients who achieved remission at the end of treatment maintained that remission throughout the year.
Several factors influence how long results last. Patients who achieve full remission during the initial course tend to stay well longer than those who only partially improve. A shorter history of depression, fewer prior medication failures, and younger age are all associated with more durable results. Combining TMS with psychotherapy and healthy lifestyle habits also extends the benefits.
If symptoms do start to return, maintenance TMS sessions or a short booster course of three to six treatments is usually enough to recapture symptom control. TMS is not a one-and-done cure, but for many patients, it provides lasting relief that medications alone could not deliver.
Do You Have to Do TMS Forever?
No, you do not have to do TMS forever. A standard course of TMS treatment runs four to six weeks of daily sessions. After that, most patients do not need ongoing treatment. Research shows that about two-thirds of patients maintain improvement for six to twelve months after completing their initial course. Some patients never need retreatment at all.
For those who do experience a return of symptoms, a short booster series is typically effective. The goal is not lifelong treatment but rather building a strong foundation of brain health that you can maintain with therapy, healthy habits, and periodic check-ins with your provider.
What Does TMS Feel Like?
TMS feels like a tapping or clicking sensation on the scalp where the magnetic coil is placed. Most patients describe it as mildly uncomfortable at first but tolerable, and the sensation often becomes less noticeable as treatment progresses. There is no pain inside the brain because the magnetic pulses target nerve cells without affecting surrounding tissue.
Cleveland Clinic notes that TMS is a pain-free, noninvasive treatment and that the most common side effect is a mild headache during or after the session, which typically goes away on its own. Yale Medicine adds that some patients experience discomfort at the scalp site, but this usually improves after the first few sessions. You are fully awake during treatment, and many patients read, listen to music, or simply relax.
The risk of serious side effects is very low. According to UCLA Health, the risk of seizure is about one in 30,000 treatments. No seizures have occurred in the over 10,000 treatments per year administered at the UCLA TMS center. TMS is considered as safe as having an MRI, according to Yale Medicine.
Is 20 Sessions of TMS Enough?
Twenty sessions of TMS is often enough to see meaningful improvement, but a full standard course typically includes 30 to 36 sessions. A phase IV study of Deep TMS published in the Journal of Clinical Psychiatry found that patients who received 20 sessions had a 69.2% response rate and 42.1% remission rate. Those numbers increased to a 79.4% response rate and 60.3% remission rate for patients who completed 30 sessions.
The difference between 20 and 30 sessions is significant. The additional sessions allow more time for the brain to consolidate the changes TMS creates, which leads to deeper and more lasting improvement. Most providers recommend completing the full course whenever possible, and insurance typically covers the standard 30 to 36 session protocol.
TMS Therapy vs. Other Depression Treatments
TreatmentResponse RateSide EffectsAnesthesia RequiredSession LengthTMS Therapy50-80% (varies by protocol)Mild scalp discomfort, headacheNo20-40 min, 5 days/week for 4-6 weeksSSRIs / SNRIs40-60%Weight gain, sexual dysfunction, nausea, fatigueNoDaily medication; 2-8 weeks to take effectECT (Electroconvulsive Therapy)70-90%Memory loss, confusion, muscle sorenessYes (general)5-10 min under anesthesia; 2-3x/weekSpravato (Esketamine)Rapid onset for some patientsDissociation, dizziness, nausea; 2-hour monitoringNo (supervised nasal spray)2+ hours per visit including monitoringCBT (Psychotherapy)Comparable to medication for mild-moderate depressionNone (psychological discomfort possible)No45-60 min, weekly for 12-20 sessions
Sources: Harvard Health; Cureus; AAFP; APA Clinical Practice Guideline; Johns Hopkins Medicine; Yale Medicine; NIMH
Who Is a Good Candidate for TMS Therapy?
A good candidate for TMS therapy is an adult who has been diagnosed with major depressive disorder and has not found adequate relief from at least one antidepressant medication. TMS is also FDA-cleared for obsessive-compulsive disorder (OCD). You may be a strong candidate if you have experienced unwanted side effects from medications or if you prefer a non-drug, non-invasive approach to treatment.
TMS is not recommended for people with metal implants in or near the head (such as cochlear implants or aneurysm clips), a history of seizures or epilepsy, or certain other neurological conditions. Cleveland Clinic provides a detailed list of contraindications. A thorough mental health evaluation before starting treatment helps determine whether TMS is safe and appropriate for you.
Treatment-resistant depression affects about 30% of people with major depressive disorder, according to Johns Hopkins Medicine. That is roughly one in three people with depression who need something beyond standard medication. For those patients here in the Miami Lakes area, we offer NeuroStar TMS therapy as a clinically proven option.
Does TMS Help With Anxiety?
Yes, TMS can help with anxiety, especially when anxiety occurs alongside depression. A 2021 research review found that TMS may reduce overactivity in the prefrontal cortex, which is a pattern commonly seen in people with anxiety. Healthline reports that as TMS treats depression and OCD, it often eases anxiety symptoms as well, because these conditions frequently overlap.
One study found that 11 out of 13 patients with generalized anxiety disorder (GAD) showed a positive response to TMS, with the majority achieving remission. While TMS is not yet FDA-approved specifically for anxiety as a standalone condition, the clinical evidence is promising, and many patients report significant anxiety relief as a secondary benefit of their depression treatment. If anxiety is a major concern, anxiety treatment that combines TMS with therapy and medication management can address both conditions at once.
Can TMS Be Combined With Other Treatments?
Yes, TMS can be combined with other treatments, and doing so often produces better outcomes. Research shows that patients who combine TMS with antidepressant medication have a relapse rate of about 16% at 12 months, compared to roughly 44% for medication alone. Adding cognitive behavioral therapy (CBT) to a TMS protocol has also been shown to improve response and remission rates.
At our practice, we frequently combine TMS with medication management and psychotherapy because we believe a multi-layered approach gives patients the strongest foundation for lasting recovery. TMS addresses the brain's circuitry. Therapy builds coping skills. Medication provides additional chemical support when needed. Together, they cover more ground than any single treatment alone.
Frequently Asked Questions
Does TMS Reset Your Brain?
TMS does reset your brain in the sense that it restores normal activity in brain regions that have become underactive due to depression. UT Southwestern Medical Center describes TMS as a treatment that can effectively reset dysfunctional brain patterns. It increases neuroplasticity, which is the brain's ability to form new neural pathways, allowing patients to break free from the depressive cycle. It does not erase memories, change your personality, or alter who you are.
Can You Do Two TMS Sessions in One Day?
Yes, it is possible to do two TMS sessions in one day under certain accelerated protocols. UT Southwestern Medical Center has developed an inpatient program that delivers up to 10 treatments per day, completing a full course in just five days. However, standard outpatient TMS uses one session per day, five days per week, for four to six weeks. Your provider will determine the right protocol based on your condition and clinical needs.
What to Do Next if TMS Does Not Work?
If TMS does not work after a full course of treatment, there are still other options. These include switching to a different TMS protocol, trying Spravato (esketamine), electroconvulsive therapy (ECT), or adjusting your medication and therapy plan.
Johns Hopkins Medicine notes that newer advancements in treatment-resistant depression therapies continue to expand the options available. A depression that has not responded to one approach does not mean it cannot be treated.
How Do I Know if TMS Is Working?
You know TMS is working when you notice gradual improvements in sleep, energy, focus, and interest in daily activities. Your provider will also track your progress using standardized tools like the PHQ-9 depression scale at regular intervals throughout treatment. UCLA Health research found that early improvements within the first five to ten sessions are strong predictors of overall treatment success.
Can You Take a Week Off of TMS?
Taking a week off of TMS is generally not recommended during the active treatment phase because consistency is important for building momentum in the brain. Missing sessions can reduce the effectiveness of the treatment. However, brief interruptions of a day or two are usually manageable. If you need to take time off, discuss it with your provider so they can adjust your schedule accordingly.
Is TMS Covered by Insurance?
Yes, TMS is covered by most major insurance plans for the treatment of major depressive disorder when the patient has not responded to at least one antidepressant medication. Medicare also covers TMS therapy. Coverage specifics vary by plan, so it is important to verify your benefits before starting treatment. New patients can reach out to our team for help with insurance verification.
Does TMS Increase Anxiety?
TMS does not typically increase anxiety. In fact, many patients experience reduced anxiety as a secondary benefit of treatment. Some patients may feel mild nervousness before their first session, which is a normal reaction to any new medical procedure. If you already deal with anxiety, letting your provider know helps them adjust the treatment environment to keep you comfortable.
The Takeaway
TMS therapy offers a proven, drug-free, non-invasive option for people with depression who have not found relief through medication alone. The benefits are backed by extensive research: improved mood, better sleep, sharper focus, and results that can last months to over a year. It is safe, well-tolerated, and can be combined with therapy and medication for even stronger outcomes.
If you have been living with depression that will not budge, or if medication side effects have made treatment feel like a trade-off, TMS may be the next step worth exploring. South Florida Med Group offers NeuroStar TMS therapy alongside psychiatric care, psychotherapy, and Spravato, so you have access to a full range of advanced treatment options in one place.
Call us at (786) 860-8844 to schedule a consultation and find out if TMS is right for you.

.png)
.png)
.png)



.png)
.png)
.png)



.png)

.png)
